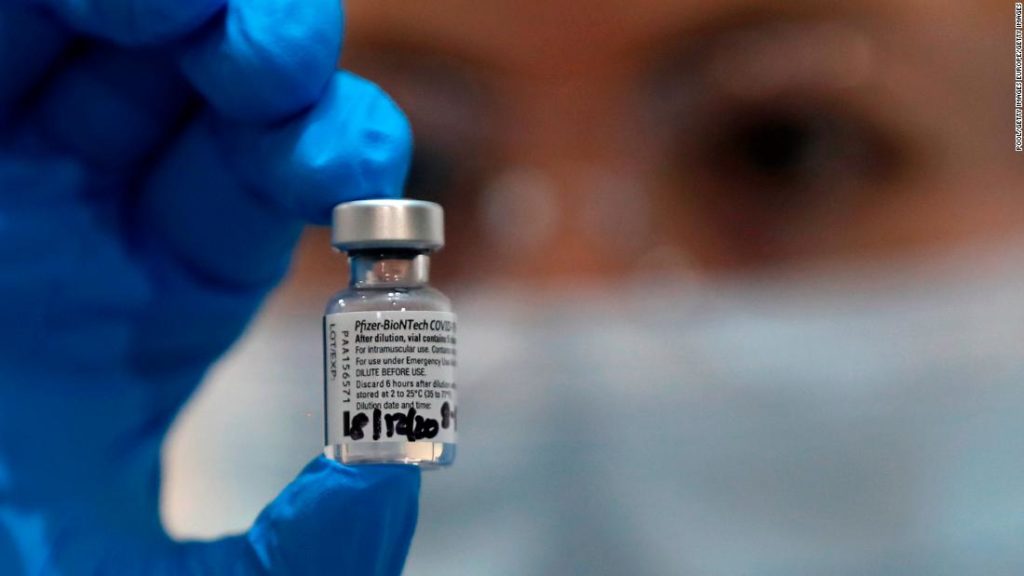
“The FDA’s authorization for emergency use of the first COVID-19 vaccine is a significant milestone in battling this devastating pandemic that has affected so many families in the United States and around the world,” FDA Commissioner Dr. Stephen Hahn said in a statement.
“Today’s action follows an open and transparent review process that included input from independent scientific and public health experts and a thorough evaluation by the agency’s career scientists to ensure this vaccine met FDA’s rigorous, scientific standards for safety, effectiveness, and manufacturing quality needed to support emergency use authorization.
“The tireless work to develop a new vaccine to prevent this novel, serious, and life-threatening disease in an expedited timeframe after its emergence is a true testament to scientific innovation and public-private collaboration worldwide.”
Before vaccinations can begin, a US Centers for Disease Control and Prevention immunization advisory committee still must vote to recommend the vaccine, and the CDC must accept that recommendation.
The Advisory Committee on Immunization Practices was scheduled to meet Saturday morning.
But until many more are vaccinated, mitigation efforts such as wearing masks and keep a safe distance need to continue to stop the virus from spreading.
How the vaccine works
Pfizer and BioNTech’s coronavirus vaccine, called BNT162b2, is an mRNA vaccine given as two shots administered 21 days apart. One dose is to prime the body, and then a few weeks later, the second dose is to boost the response.
The messenger RNA or mRNA used in the vaccine codes for a structure called the spike glycoprotein of the virus. That’s the part of the virus that it uses to attach to cells. The vaccine prompts the human body to produce copies of that protein, eliciting an immune response that leads to some protection against coronavirus infection.
Such mRNA vaccines are the newest approach to vaccine technology.
The data come from more than 43,000 trial participants: 21,720 who were randomly given the vaccine and 21,728 who were randomly given a placebo. The data show that there were only eight Covid-19 cases among people who received the vaccine, compared with 162 cases among those given the placebo.
However, FDA briefing documents also note that the vaccine appears to provide “some protection” against Covid-19 following just one dose.
The documents describe the efficacy of Pfizer’s vaccine in the time between the first and second dose as 52.4%, but the document notes that “the efficacy observed after Dose 1 and before Dose 2, from a post-hoc analysis, cannot support a conclusion on the efficacy of a single dose of the vaccine, because the time of observation is limited by the fact that most of the participants received a second dose after three weeks.”
In other words, “the trial did not have a single-dose arm to make an adequate comparison.”
The document goes on to detail the safety profile of the vaccine as “favorable” and notes that the most common adverse reactions to the vaccine have been reactions at the injection site, fatigue, headache, muscle pain, chills, joint pain and fever.
Severe adverse reactions occurred in less than 4.6% of participants, were more frequent after the second dose and were generally less frequent in older adults as compared to younger participants, according to the document. The document adds that swollen lymph nodes also may be related to vaccination.
Overall, “there are currently insufficient data to make conclusions about the safety of the vaccine in subpopulations such as children less than 16 years of age, pregnant and lactating individuals, and immunocompromised individuals,” according to the document.
In the advisory committee’s Thursday meeting, FDA official Dr. Marion Gruber said the fact sheet and prescribing information provided with Pfizer’s Covid-19 vaccine will warn that people with a history of severe allergic reactions to any of the vaccine’s components should not get it.
Vaccine distribution to begin soon
In most cases, the first shipments of the vaccine will be transported from Pfizer’s facility in Kalamazoo, Michigan, to hospital systems and pharmacies.
The distribution from vaccine production company to individual hospitals and pharmacies in each state as directed by the federal government, is different for almost every state. State health department officials are coordinating with federal officials in Operation Warp Speed. However, there is no clear roadmap that explains how this process is working simultaneously in all 50 states.
Instead, states have developed individualized vaccine distribution plans that vary slightly for each individual state’s demographic and geographic needs.
CDC officials have been in close contact with state leaders about how their distribution plans will work and challenges that could crop up state to state.
You may also like
-
UK coronavirus variant has been reported in 86 countries, WHO says
-
NASA technology can help save whale sharks says Australian marine biologist and ECOCEAN founder, Brad Norman
-
California Twentynine Palms: Explosives are missing from the nation’s largest Marine Corps base and an investigation is underway
-
Trump unhappy with his impeachment attorney’s performance, sources say
-
Lunar New Year 2021: Ushering in the Year of the Ox