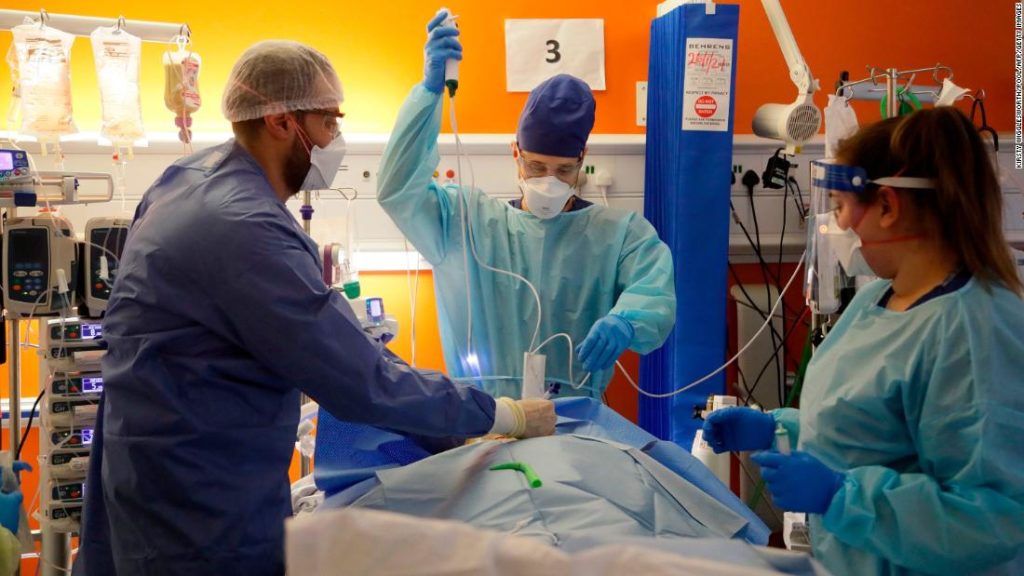
Scientists are not surprised to see the coronavirus changing and evolving — it’s what viruses do, after all. And with so much unchecked spread across the US and other parts of the world, the virus is getting plenty of opportunity to do just that.
Four of the new variants are especially worrisome.
“The variants that have been identified recently seem to spread more easily. They’re more transmissible, which can lead to increased number of cases, and increased stress on our already overtaxed system,” Dr. Rochelle Walensky, the newly appointed director of the Centers for Disease Control and Prevention, said in a briefing Wednesday.
What scientists most fear is that one will mutate to the point that it causes more severe disease, bypasses the ability of tests to detect it or evades the protection provided by vaccination. While some of the new variants appear to have changes that look like they could affect immune response, it’s only by a matter of degree.
Governments are already reacting. Colombia banned flights from Brazil, and Brazil banned flights from South Africa. It’s almost certainly too late to stop the spread, and there’s some indication the mutations in these variants are arising independently and in multiple places.
Here’s what’s known about the top four.
B.1.1.7
At the top of the list for researchers in the US is the B.1.1.7 variant first seen in Britain. The CDC has warned it could worsen the spread of the pandemic. It reports more than 300 cases in 28 states — but those are only the cases caught by genomic sequencing, which is hit and miss in the US.
Although hearing about mutant new viruses can frighten people, scientists say they are reassured by what they have found: The human immune system can handle the variants that have sprung up so far, especially B.1.1.7.
“As far as we know it is transmitted in exactly the same way,” Gregory Armstrong, who directs the Office of Advanced Molecular Detection at CDC, told CNN.
That means the same measures already known to reduce spread will also stop the new variants: mask use, social distancing, avoiding large groups or crowds and frequent handwashing.
However, the mutations in the variant help it enter cells more easily — which means if someone, says, breathes in a lungful of air that has virus particles in it, those particles are going to be more likely to infect some cells in the sinuses or lungs rather than bouncing off harmlessly. The worrisome changes enhance the spike protein that the virus uses to attach to cells, meaning people are more likely to become infected by an exposure.
So people need to try harder to prevent spread until vaccination can be sped up.
“In order to interrupt transmission, we are going to need higher rates of what we do to slow transmission,” Armstrong said. “We are going to need to pay more attention to wearing masks. And we will need to increase vaccine coverage.”
There have been some confusing reports about whether B.1.1.7 has caused more severe disease in Britain.
“The most recent data indicate from the UK that it appears to be a bit more virulent in the sense of potentially causing more serious disease,” National Institute of Allergy and Infectious Diseases Director Dr. Anthony Fauci told a webcast Thursday sponsored by the National Education Association.
B.1.351
The variant first seen in South Africa called B.1.351 or 501Y.V2 was reported for the first time in the US Thursday, in South Carolina.
The two people lived in different parts of the state and neither had traveled recently, although Dr. Brannon Traxler, the health department’s interim public health director, declined to say whether that indicated the variant must be spreading in the community.
It’s been seen in more than 30 other countries, according to the World Health Organization.
“The variant which was first detected in South Africa has spread quickly beyond Africa and so what’s keeping me awake at night right now is that it’s very likely circulating in a number of African countries,” Dr. Matshidiso Moeti, WHO regional director for Africa, said Thursday.
It has a different pattern of mutations that causes more physical alterations in the structure of the spike protein than B.1.1.7 does. One important mutation, called E484K, appears to affect the receptor binding domain — the part of the spike protein most important for attaching to cells.
It could help the virus partly escape the effects of vaccines. “There is more concern about immune escape,” Armstrong said. Vaccine makers and academic researchers are testing samples of this variant, along with others, to see if it can evade the immune response caused by vaccination.
Fauci says even so, there’s an extra cushion of immunity caused by vaccination. It gives some wiggle room. “The good news is the vaccines as they exist now still would be effective against the mutants. The sobering news … as you get more and more replication, you can get more and more of evolution of mutants, which means you always got to be a step ahead of it,” Fauci told CNN on Monday.
“For sure there is a breadth of different kinds of antibodies that can neutralize the virus. These kinds of things in plasma are likely to be resistant to the emerging mutations,” said Dr. Michel Nussenzweig of Rockefeller University, who’s been testing out different mutations against the blood of people who have been vaccinated.
Teams at Columbia University, the Aaron Diamond AIDS Research Center at Columbia University and elsewhere have also been testing lab-made versions of the viral mutations against the blood of vaccinated people and say while there does seem to be a somewhat diminished effect of vaccination, its not enough to weaken protection — yet.
Just in case, Pfizer and Moderna are working to make booster vaccines that would address mutant versions. The design of the vaccines is meant to make that a quick and easy process — just plugging in a new version of the genetic code used to generate the vaccines will do it.
There’s also evidence the changes may help some escape from monoclonal antibody treatments made by Eli Lilly and Co. and Regeneron, also.
P.1
A variant suspected of fueling a resurgence of viral spread in Brazil turned up in Minnesota for the first time this week. It was in a traveler from Brazil, so there’s no indication yet of community spread.
This variant, called P.1, was found in 42% of specimens in one survey done in the Brazilian city of Manaus, and Japanese officials found the variant in four travelers from Brazil.
“The emergence of this variant raises concerns of a potential increase in transmissibility or propensity for SARS-CoV-2 re-infection of individuals,” the CDC said. P.1 also carries the E484K mutation.
L425R
Finally, there’s a new variant seen in California, as well as a dozen other states. “We don’t know yet what the significance of that one is,” said Armstrong. It also has a mutation in the receptor binding domain of the spike protein. It is called L425R and while it’s being found commonly, it’s not yet clear if it’s more transmissible.
Any viral strain can become more common because of what’s known as the founder effect. “The founder effect is a matter of a virus being in the right place at the right time,” Armstrong said. If a particular strain happens to be circulating when transmission increases because of human behavior, that strain will ride along and become more common not because it spreads more easily, but simply because it was there.
It will take more study to show whether these variants can increase the already astronomical spread of the virus. The US has more than 25 million diagnosed cases and more than 430,000 deaths.
“The emergence of variants underscores the need for public health action,” Walensky advised.
“First, get vaccinated when it’s your turn. Also, some people may need help getting vaccinated — please consider helping your neighbors and loved ones schedule or travel to their appointments. Second, wear a mask. Practice social distancing and wash your hands. And finally, now is not the time to travel.”
You may also like
-
UK coronavirus variant has been reported in 86 countries, WHO says
-
NASA technology can help save whale sharks says Australian marine biologist and ECOCEAN founder, Brad Norman
-
California Twentynine Palms: Explosives are missing from the nation’s largest Marine Corps base and an investigation is underway
-
Trump unhappy with his impeachment attorney’s performance, sources say
-
Lunar New Year 2021: Ushering in the Year of the Ox