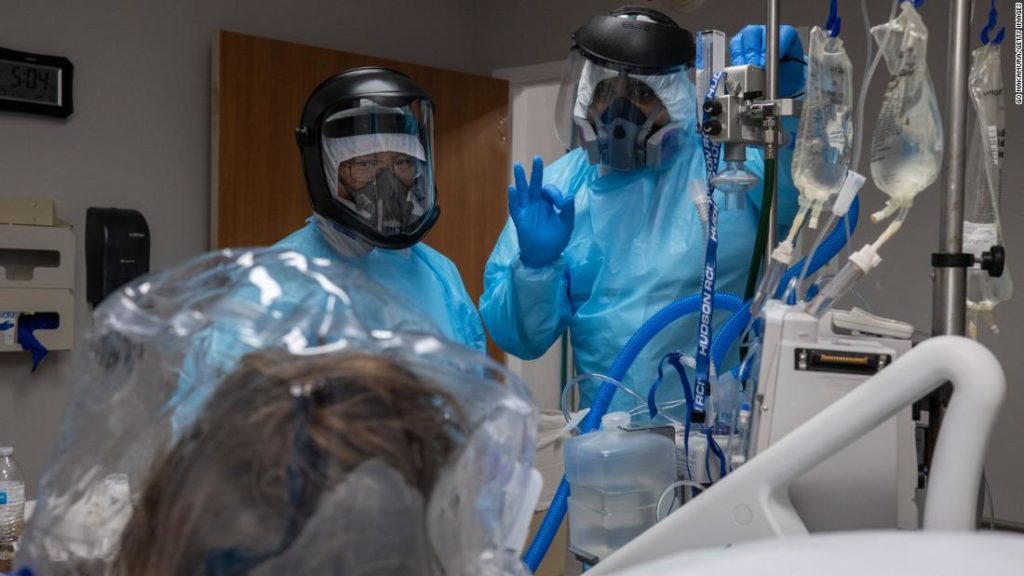
“Say, ‘I’m not going to be one of the people that’s going to be a steppingstone for the virus to go to somebody else. I’m going to be a dead end to the virus,'” Fauci told Facebook CEO Mark Zuckerberg Monday.
Holiday gatherings — like Thanksgiving and upcoming Christmas and Hanukkah — are the “perfect setup” for people who have no symptoms to “innocently and inadvertently” spread infections to their loved ones.
With that in mind, officials are preparing for the first wave of vaccine distributions.
Stephen Hoge, the president of Moderna, told NBC’s Lester Holt on Monday that they are “quite optimistic” when it comes to authorization of their Covid-19 vaccine candidate.
“We are quite optimistic, actually, that the vaccine is — the data speaks for itself and they’ll be supportive,” Hoge said in a preview clip from a longer interview, set to air on “Dateline” Thursday night.
Once the US Food and Drug Administration grants EUAs and the US Centers for Disease Control and Prevention makes recommendations on which groups will get the vaccines first, they will be ready to be shipped out, Dr. Moncef Slaoui, Operation Warp Speed chief scientific adviser, said Monday. And that very day or the next, the first immunizations can be administered, he said.
Panel debates who gets vaccines first
Two Covid-19 vaccines are expected to be ready by the end of the month, and already one thing is clear: There won’t be enough vaccines to go around.
“This is an unprecedented vote that ACIP will be making,” said Dr. William Schaffner, a member of the panel since 1982.
Vaccinations are expected to begin in mid- to late December, depending on other approvals. The panel is set Tuesday to vote on whether the first group to be vaccinated should be health care workers and residents of nursing homes.
If those two groups are first — or “Phase 1a” in CDC parlance — then other high priority groups will have to wait, including people with underlying medical conditions, essential workers such as police officers and firefighters, and elderly people who are not in nursing homes.
ACIP chair Dr. Jose Romero said to expect frontline health care workers to get the first wave of vaccines.
“It seems pretty clear that the top group of individuals will be health care providers,” Romero told CNN’s New Day.
Each state will then decide who within that group of providers will get the vaccine first.
“Anybody that works within a health care institution that could have contact with an individual who has Covid should receive vaccination,” Romero added. “That includes individuals such as the persons delivering food, those persons in housekeeping who rapidly turn over rooms in the emergency room or who perform cleaning in the patient’s rooms. Those individuals will be included.”
US still battling a surge
But even after vaccines start to be distributed in December, there won’t be enough for the wider public to be immunized until April or May of 2021, Fauci said. Until then, the US is still contending with an unprecedented spike.
In Minnesota, more than a third of counties are 10 times over what would be considered a high-risk threshold for infection rate growth as the state is in “the worst spot we’ve been in since March,” Minnesota Department of Health Commissioner Jan Malcolm said Monday.
“When there’s this great increase in the number of Minnesotans needing hospitalization for Covid, that can have some really serious implications for the availability of hospital care for other critical issues as well,” Malcolm said. “And the number of people being admitted for Covid is far overshadowing what we saw back in May.”
At least 35 hospitals in Minnesota are reporting over 95% of their staffed ICU beds are in use, according to the state’s dashboard.
To manage the risk of reopening, New Mexico Gov. Michelle Lujan Grisham announced a new “Red to Green” system that tiers counties by their risk of spread. The data will be updated biweekly, and if a county fails to meet the metrics, it will begin operating at the most restrictive level within 48 hours.
Nationally, Monday marked the 28th consecutive day that the US reported more than 100,000 new cases — a number that far exceeds the records set in the spring and summer surges which both stayed below 60,000.
Hospitals under stress
As cases increase over the holiday season, so have hospitalizations — putting health care systems under stress.
California Gov. Gavin Newsom on Monday told reporters that the intensive care unit bed capacity in the state might reach 112% by Christmas Eve, if the trend of surging coronavirus cases continues.
In Rhode Island, officials have prepared to use field hospitals after telling residents their systems were already at capacity.
In New York, where some hospitals saw room capacity taxed in March, Gov. Andrew Cuomo said this time medical systems need to take steps to move patients to other facilities that have space.
“No patient wants to be in an overwhelmed hospital, because you’re getting less care, the staff is stretched thin, it’s in the patient’s best interest, distribute the patient load over the system,” Cuomo said Monday. “We’re not going to live through the nightmare of overwhelmed hospitals again.”
Health care systems might be even more strained this time around because researchers are now seeing people affected by the virus even after they no longer show symptoms, Fauci said.
Some, called “long haulers,” experience lingering symptoms for months. Others see residual and perhaps indefinite organ system dysfunction, he said.
“The idea that you get infected, you either get no symptoms or you die, and if you don’t die, you’re OK — I think that’s really a misperception,” he added.
Challenges for small communities to get vaccines
Health care systems already under stress will face another challenge distributing vaccines to rural communities, experts say.
Pfizer has planned its vaccine to be in ultracold storage and shipped in thermal shippers that can hold at least 975 and up to 5,000 doses.
“That’s not workable from a small town, rural perspective,” Alan Morgan, chief executive officer of the National Rural Health Association, told CNN Monday. “It just isn’t.”
Those doses will have to be broken up among multiple providers in those communities, and they will have to do it without risking the temperature at which they are stored, Hannan said,
Immunization managers in those areas are going to have to find solutions like having providers pick up doses from a central location or shipping them out in containers with dry ice, Morgan and Hannan said.
If they don’t, they risk being sidelined, said Morgan.
“That type of approach just sets up these rural communities across the US for really unacceptable mortality rates and the potential for the collapse of the health care system,” he said.
Pfizer did not have an immediate response questions about the concerns over shipment sizes.
CNN’s Elizabeth Cohen, Maggie Fox, Lauren Mascarenhas, Raja Razek, Steve Almasy, Holly Yan, Sara Murray, John Bonifield, Shelby Lin Erdman and Jennifer Selva contributed to this report.
You may also like
-
UK coronavirus variant has been reported in 86 countries, WHO says
-
NASA technology can help save whale sharks says Australian marine biologist and ECOCEAN founder, Brad Norman
-
California Twentynine Palms: Explosives are missing from the nation’s largest Marine Corps base and an investigation is underway
-
Trump unhappy with his impeachment attorney’s performance, sources say
-
Lunar New Year 2021: Ushering in the Year of the Ox