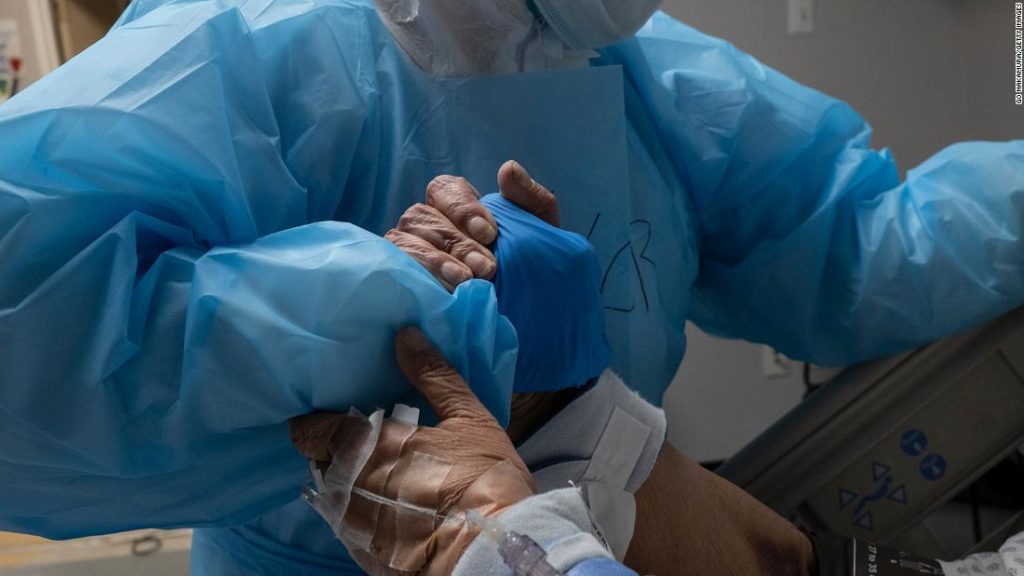
But for much of the US, the pandemic is raging out of control — and will get worse before everyone can be vaccinated.
In just the past week, more than 18,000 people died from Covid-19 in the US. Hospitals are filling up fast.
And the US set a record Friday for the most Covid-19 infections reported in one day: 249,709, according to Johns Hopkins University.
“Unfortunately, it will get worse because we still are experiencing the outcome of the Thanksgiving holiday and gatherings,” said Moncef Slaoui, chief scientific officer for Operation Warp Speed, the federal government’s vaccine initiative.
“And unfortunately, there may be more over the Christmas holiday. So there will be a continuing surge.”
More than 2 million travelers were screened at US airports between Friday and Saturday, the Transportation Security Administration said.
Where the Moderna vaccine will likely go
The first public doses of the Moderna vaccine will “most likely” be administered Monday morning, Slaoui said.
Distribution of the Moderna vaccine has already started, said Army Gen. Gustave Perna, chief operating officer of Operation Warp Speed.
Just like the Pfizer/BioNTech vaccine, the Moderna vaccine has received emergency use authorization from the US Food and Drug Administration.
More than 6 million doses of Moderna’s vaccine will be shipped to more than 3,200 sites where they will be administered — far more than the 636 sites that Pfizer’s vaccines were shipped to.
As for the Pfizer/BioNTech vaccine, more than 272,000 doses had been administered as of Saturday, according to the CDC.
Recipients of either vaccine must get two doses. The Pfizer/BioNTech doses should be spaced 21 days apart, and the Moderna vaccine should be spaced 28 days apart.
Excitement about a second vaccine must be tempered by a huge caveat: Only high-priority groups (such as health care workers and residents of long-term care facilities) will get vaccinated first.
But now we have an idea of who could receive vaccines next.
The CDC’s advisory committee voted Sunday afternoon to prioritize older adults ages 75 and older and frontline essential workers in the next phase of vaccine allocation.
For the subsequent phase, the committee voted to prioritize adults between the ages of 65 and 75, people between the ages of 16 and 64 with high-risk medical conditions, and other essential workers.
These recommendations will “serve to address the current lack of vaccine supply and address those individuals with the highest risk for disease,” said Dr. José Romero, the chair of the committee and the secretary of the Arkansas Department of Health.
Slaoui believes vaccines will still be effective after virus variation
But “up to now, I don’t think there has been a single variant that would be resistant to the vaccine,” Slaoui sad. “We can’t exclude it, but it’s not there now.”
He said the novel coronavirus may be prone to variance. But critical aspects of the virus, such as the spike protein involved in a vaccine, are very specific to the novel coronavirus and unlikely to mutate much.
“Because the vaccines are using antibodies against many different parts of the spike protein, the chances that all of them change, I think, are low,” Slaoui said.
Most Americans will still have to wait months for a vaccine
By the end of this year, “we will have enough doses to vaccinate nearly 20 million people,” said Dr. Amanda Cohn, executive secretary for the CDC’s Advisory Committee on Immunization Practices.
“By the end of January, we will have enough doses to vaccinate nearly 30 million additional people, and then by the end of February, 50 million additional people,” Cohn said Sunday.
In other words, most Americans won’t be able to get a Covid-19 vaccine until sometime in 2021.
Dr. Carlos del Rio, executive associate dean of Emory University’s School of Medicine, said he agreed with that assessment.
“We’re just simply saying, ‘Well, we’re getting vaccine.’ But the vaccine is coming way too late for thousands of people who will die before we get the vaccine distributed widely,” del Rio said Thursday.
“Transmissions (of the virus) are actively happening, and I think before the end of the year, we may be getting close to 4,000 deaths a day,” del Rio said.
As for when children might be able to receive the vaccine, Moderna has an ongoing study of its vaccine in adolescents between the ages of 12 and 18. The company is also discussing an additional clinical trial for children between the ages of 6 months and 12 years with the National Institutes of Health.
CDC gives new advice for those with a history of allergic reactions
After several reports of allergic reactions to the Pfizer/BioNTech vaccine, the CDC now suggests those who have ever had a severe allergic reaction to an ingredient in a Covid-19 vaccine should not get that vaccine and should consult a doctor.
A reaction is considered severe if it requires the person to be treated with epinephrine, or they need to be hospitalized. Such reactions can include shortness of breath, a closing of the throat, nausea and dizziness.
If someone gets a severe allergic reaction after the first dose of a Covid-19 vaccine, they should not get the second dose, the CDC said.
Those who have severe allergies unrelated to vaccines or injectable medications can still get a Covid-19 vaccines, the agency said.
The CDC also said those who have a history of allergies to any oral medications or people with milder reactions to vaccines can also still get vaccinated.
Vaccine providers should monitor all people for 15 minutes after getting the vaccine for any possible reaction, and those with a history of severe allergic reactions should be monitored for 30 minutes, the CDC said.
It said all vaccine providers should have epinephrine, antihistamines, stethoscopes, blood pressure cuffs and timing devices on hand to treat and monitor reactions.
But so far, the percentage of vaccine recipients who had a severe reaction is extremely low.
Of the 556,208 Pfizer/BioNTech doses given as of Sunday, only a handful serious allergic reactions have been reported.
Several health care workers at Providence Health Alaska suffered adverse reactions, spokesman Mikal Canfield said Saturday. The reactions were not life-threatening.
In total, five people in Alaska had adverse reactions across the state.
In suburban Chicago, adverse reactions in four employees caused a hospital to temporarily stop its Covid-19 vaccination program for frontline workers.
The health care company noted those four workers represented “fewer than 0.15% of the approximately 3,000 who have so far received vaccinations across Advocate Aurora Health.”
The health care system said the program will resume Sunday, but with increased time to monitor people after getting the vaccine.
US Surgeon General Dr. Jerome Adams said allergic reactions to vaccines are “not abnormal or unexpected.”
“The system is working,” Adams said. “We are recognizing and catching these very, very rare side effects.”
CNN’s Nadia Kounang, Jacqueline Howard, Ben Tinker, Arman Azad, Virginia Langmaid, Lauren Mascarenhas, Paul Vercammen, Pete Muntean and Gisela Crespo contributed to this report.
You may also like
-
UK coronavirus variant has been reported in 86 countries, WHO says
-
NASA technology can help save whale sharks says Australian marine biologist and ECOCEAN founder, Brad Norman
-
California Twentynine Palms: Explosives are missing from the nation’s largest Marine Corps base and an investigation is underway
-
Trump unhappy with his impeachment attorney’s performance, sources say
-
Lunar New Year 2021: Ushering in the Year of the Ox